One of the hardest roles of the emergency physician is giving bad news to a patient or their family members. Difficult topics that are often challenging for physicians to discuss include reporting the death of a family member or giving the diagnosis of a terminal illness. The optimal way to relay these topics is yet to be determined and each practitioner typically develops their own communication style. Some choose to deliver the message in a direct and succinct manner while others prefer a more drawn out and complete explanation. The Emergency Department provides a unique environment as there is often little time to develop any rapport with the patient and their family. This can make communicating these topics more challenging. In addition, breaking bad news involves more than just the verbal component of actually giving the bad news. It also requires the ability to respond effectively to patient’s and family’s emotional reactions and the dilemma of how to give hope when the situation is bleak.
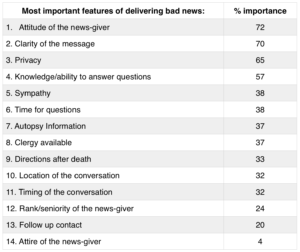
Jurkovich et al studied the characteristics and methods of delivering bad news from the perspective of surviving family members. The chart below details the importance of various elements rated by respondents in the study. The attitude and clarity of the message delivered by the provider were deemed to be most important, while the attire of the provider had little importance to the respondents.
The duty of breaking bad news can be improved by understanding these characteristics and methods and then applying a step-wise method to effectively communicate and counsel patient’s and/or their families. In a recent Wednesday conference, Dr. Flannery, one of our core faculty attendings, introduced us to the SPIKES protocol for breaking bad news. The purpose of the protocol is to help the clinician fulfill the essential goals of gathering information, providing intelligible information, and supporting the patient or family by reducing their emotional impact and isolation. When we are informing our patients of an unfortunate diagnosis, the protocol also calls for collaborating in developing a strategy or treatment plan for the future. From the Emergency Department standpoint, this means guiding patients to the correct consultant for further workup and treatment options.

During our Wednesday conference, we broke into small groups and practiced situations that would be considered difficult to give bad news. The experience was positive and allowed us to give each other constructive criticism on ways to improve our approach to giving bad news. As a senior resident, I have unfortunately been involved in many of these situations throughout my residency. I have learned that despite the challenges involved in delivering bad news, there is also tremendous gratification in providing a therapeutic presence during a patient or family’s greatest need.
References:
1. Jurkovich et al. Giving bad news: the family perspective. J Trauma. May 2000
2. Baile W.F. et al. SPIKES – A Six-Step Protocol for Delivering Bad News: Application to the Patient with Cancer. The Oncologist. June 12, 2000.
