Resident: D’Amore/Clayton
CC: “My heart is racing.”
HPI: 26 year old male with no past medical history presents to the Emergency Room with complaints of palpitations. Patient states that while exercising at the gym just prior to arrival, he suddenly developed palpitations along with associated lightheadedness. He reported one similar episode in the past that self-remitted. He denies chest pain, shortness of breath, nausea or vomiting but was experiencing intermittent lightheadedness. He denies taking any medication prior to arrival. Patient states he drinks ETOH infrequently with his last drink several days ago. He denies tobacco or illicit drug use. Patient also denies any family history of heart disease or arrhythmias.
Physical Exam:
Vitals: HR: 221 BP: 117/74 RR: 20 T: 98.8 Pulse Ox 100% on Room Air
General: Patient is awake, appears uncomfortable
Respiratory: No respiratory distress. Lungs are clear to auscultation.
Cardiovascular: +S1/+S2, tachycardic, irregular. No murmurs, rubs or gallops.
Abdomen: Soft, non-tender, non-distended
Extremities: Palpable, rapid pulses. No cyanosis, clubbing, or edema.
Neurological: Alert and oriented to person, place, time, and situation, following all commands, strength and sensation intact and equal bilaterally.
Laboratory Data:
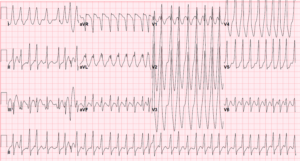
Lab work and radiography including troponins, complete blood count, complete metabolic panel, thyroid stimulating hormone, chest x-ray, and urine drug screen were all within normal limits. Image 1 is the EKG on presentation. The patient quickly became hypotensive 90/52 and complained of lightheadedness. The patient was quickly sedated and cardioverted with 150 joules. He returned to sinus rhythm at which time the underlying conduction was more apparent.
Questions
- What EKG abnormalities do you notice?
- EMS requests permission to administer 6mg of Adenosine to treat the arrhythmia.
What is your recommended treatment plan?
Answers:
- This EKG demonstrates Wolff-Parkinson-White Syndrome with Atrial Fibrillation.
- Advise EMS not to treat with Adenosine or other A-V nodal blocking agents as this may precipitate ventricular tachycardia or ventricular fibrillation.
Discussion:
Wolff-Parkinson-White Syndrome is a pre-excitation syndrome where myogenic bundles known as the Bundles of Kent directly link the atria to the ventricles, bypassing the atrioventricular (AV) node and the organized infranodal system [source: Tintinalli]. Atrial Fibrillation (AFib) in Wolff-Parkinson-White Syndrome (WPW) is a presentation of this syndrome in up to 20% of cases.
Features include an irregularly irregular rhythm, very rapid ventricular rates often in the range of 250 to 300, and widened QRS complexes that differ in duration and morphology from one to the next.The accessory pathway present in patients with WPW allow for the multitude of additional ectopic atrial impulses present in AFib to bypass the AV node and conduct to the ventricles, accounting for the unusually rapid ventricular rates. The variation in QRS duration and morphology can also be attributed to simultaneous conduction through the traditional AV node-His-Purkinje pathway as well as the Bundle of Kent-Ventricle route.
WPW with AFib is often misdiagnosed as a supraventricular tachycardia (SVT), ventricular tachycardia (VT) or atrial fibrillation with a bundle branch block, all of which can be safely treated with AV nodal blockers such as Adenosine, Diltiazem, and Amiodarone. WPW in the presence of atrial fibrillation makes degeneration into ventricular fibrillation more likely and thus synchronized cardioversion, delivering 0.5 – 2 Joules/kilogram, is the first-line treatment. Second-line treatments include Procainamide or Ibutilide whose mechanism prolongs the refractory period of the accessory pathway and whose dosing is weight-based. Stable WPW in the presence of narrow-complex SVT can be treated with the traditional vagal maneuvers, adenosine, and calcium channel- or betablockers [source: Tintinalli]. Patients with WPW should undergo ablation as this syndrome can lead to sudden cardiac death by means of ventricular fibrillation.
Take Home Pearls:
- Wolff-Parkinson-White with Atrial Fibrillation presents as an irregularly irregular tachycardia with widened QRS complexes that vary in morphology and result in ventricular rates often greater than 250.
- If the QRS complex is widened, avoid use of any AV nodal blockers as they can precipitated ventricular arrhythmias.
- Procainamide and synchronized Cardioversion are the treatment of choice for WPW with AFib.
