TRANEXAMIC ACID (TXA)
By: Hima Khamar M.D., PGY3
Tranexamic acid (TXA) has become a huge asset in the world of emergency medicine when it comes to controlling hemorrhage. The main use in the ED is in traumatic hemorrhage, but there are many other uses for TXA. In this article, I will discuss some of the other uses of TXA in the hopes that the next time you come across a patient whose hemorrhage you are unable to control with conventional methods, TXA maybe an addition to your toolbox.
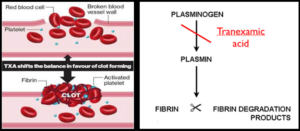
TXA is an antifibrinolytic agent. It reversibly binds plasminogen which prevents plasmin activation. Decreased plasmin activation results in inhibition of fibrin clot degradation, thereby stabilizing the clot. This increase in clot formation and stabilization is how TXA works to control hemorrhage.
TXA comes in both oral and intravenous formulations. The oral form comes in 500mg or 650mg tablets and is cheaper. The intravenous form comes in a vial that is usually 1000mg/10ml. Both of these formulations are used in different disease processes, which will be further discussed below.
Despite the many uses of TXA, there are only two indications for which it is approved: tooth extractions for hemophiliac patients (to be given prior to the procedure) and control of heavy menstrual bleeding (this is given orally on an outpatient basis). All the other uses are off label, despite many of them having great evidence.
USES OF TXA
- Traumatic hemorrhage
1g IV bolus over 10 minutes loading dose, followed by 1g IV infusion over 8 hours – MUST BE GIVEN WITHIN THE FIRST 3 HOURS.
Evidence for this came out of the CRASH 2 trial in 2010. The study concluded that TXA reduced all-cause mortality and reduced risk of death due to bleeding when compared to the placebo group. Also, the subgroup analysis showed only effective when given within 3 hours.
- Epistaxis
Topical. Soak cotton pledget or any other epistaxis control device, such as RhinoRocket in TXA prior to placing in the nostril.
Evidence for this came out of an RCT by Zahed et al. in 2017. The study showed topical TXA resulted in quicker resolution of epistaxis, decreased ED length of stay, decreased re-bleeding rate, and increased patient satisfaction when compared to placebo.
- Dental bleeding in relation to dental procedures (FDA use approved only for hemophilia patients)
Mouthwash. Create by either using 5mg of intravenous solution (1000mg/10ml) in 5ml to make 5% solution OR 650mg tablet crushed and placed in 20ml. A paste can also be created with the tablets and saline to placed directly onto the bleeding region.
Evidence for this came from multiple studies in the dental literature starting around the mid-2000s which showed TXA reduced bleeding when used in a mouth wash formulation both during the procedure and for 2-3 days after the dental procedure when compared to placebo. This was also proven in hemophilia patients and in patients on anticoagulants, such as Warfarin.
- Cyclic heavy menstrual bleeding (FDA approved use)
1300 mg PO 3x daily for up to 5 days.
Evidence for this came from multiple RCTs and is also in the ACOG guidelines for management of heavy menstrual bleeding.
- Traumatic hyphema
25 mg/kg PO 3x daily for 5-7 days.
There is not a lot of evidence for this use, but it has been looked at in small studies and it is a use recommended by the American Academy of Ophthalmology on a case by case basis. There was a study looking at topical (via drops), but the study was very small so not generalizable.
- Orthopedic and cardiac surgery
This is not in our realm, but orthopedic studies are by far the most numerous looking at various doses and various formulations to decrease intra-operative bleeding.
- Postpartum hemorrhage
1g IV bolus over 10 mins, if continues to have bleeding after 30 mins or has another re-bleed within 24 hours then give another 1g IV bolus over 10 mins. (Dosing based on study)
Evidence for this comes from the WOMAN trial published in 2017. The study concluded that “Tranexamic acid reduces death due to bleeding in women with post-partum haemorrhage with no adverse effects. When used as a treatment for postpartum haemorrhage, tranexamic acid should be given as soon as possible after bleeding onset.”
- Hemoptysis
1g of TXA in 20ml of saline nebulized over 30 mins. (Dosing is controversial)
Evidence for this is based on various case reports. No large RCT exists at this time. This is very experimental, but definitely worth a try in those post-tonsillectomy patients (including pediatrics), cancer patients (oral or lung), or any other causes of hemoptysis.
These are just some of the uses documented in the literature. I think over time we will see more uses of TXA. I have personally used it in penile bleeding secondary to a false track created by a misplaced Foley catheter. I have also used it to stop bleeding topically for varicose veins. There are also current ongoing studies looking at its use in GI bleeding as well. SO, CONSIDER TXA THE NEXT TIME YOU ARE IN A BIND.
REFERENCES:
- Bryant-Smith et al. Antifibrinolytics for heavy menstrual bleeding. Cochrane Database Syst Rev. 2018 Apr 15.
- Carter et al. Current concepts of the management of dental extractions for patients taking warfarin. Aust Dent J. 2003 Jun;48(2):89-96.
- Carter et al. Tranexamic acid mouthwash: a prospective randomized study of a 2-day regimen vs 5-day regimen to prevent postoperative bleeding in anticoagulated patients requiring dental extractions. Int J Oral Maxillofac Surg. 2003 Oct;32(5):504-7.
- Coetzee, M J. 2007. The use of topical crushed tranexamic acid tablets to control bleeding after dental surgery and from skin ulcers in haemophilia. Haemophilia. 2007 Jul;13(4):443-4.
- Hankerson et al. Nebulized Tranexamic Acid as a Noninvasive Therapy for Cancer-Related Hemoptysis. Journal of Palliative Medicine. 2015. Volume 18, Number 12, 1060-62.
- Jahadi et al. Comparison between Topical and Oral Tranexamic Acid in Management of Traumatic Hyphema. Iran J Med Sci. 2014 Mar;39(2 Suppl):178-83.
- Komura et al. Hemoptysis? Tryi inhaled tranexamic acid. The Journal of Emergency Medicine. 2018. Vol. 54, No. 5, pp. e97–e99.
- Management of acute abnormal uterine bleeding in nonpregnant reproductive-aged women. Committee Opinion No. 557. American College of Obstetricians and Gynecologists. Obstetric Gynecology 2013;121:891–6.
- Nuvvula et al. Efficacy of tranexamic acid mouthwash as an alternative for factor replacement in gingival bleeding during dental scaling in cases of hemophilia: A randomized clinical trial. Contemp Clin Dent. 2014 Jan;5(1):49-53.
- Shakur et al. Effects of tranexamic acid on death, vascular occlusive events, and blood transfusion in trauma patients with significant haemorrhage (CRASH-2): a randomised, placebo-controlled trial. Lancet 2010; 376: 23–32.
- Shakur et al. Effect of early tranexamic acid administration on mortality, hysterectomy, and other morbidities in women with post-partum haemorrhage (WOMAN): an international, randomised, double-blind, placebo-controlled trial. Lancet 2017; 389: 2105–16.
- Zahed et al. Topical Tranexamic Acid Compared With Anterior Nasal Packing for Treatment of Epistaxis in Patients Taking Antiplatelet Drugs: Randomized Controlled Trial. Academic Emergency Medicine. 2018 Mar;25(3):261-266.