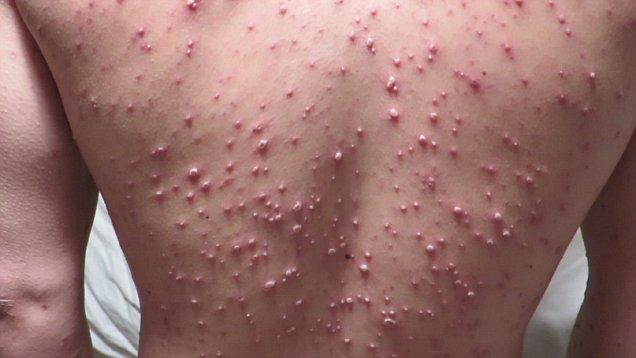
Varicella-zoster virus
Varicella (chickenpox) is a highly contagious disease caused by primary infection with varicella-zoster virus (VZV)2 and may cause maternal mortality or serious morbidity
> Reactivation of latent infection, usually many years after the primary infection, may result in herpes zoster (shingles), a painful vesicular eruption in the distribution of sensory nerve roots2
> Both varicella (chickenpox) and zoster (shingles) are notifiable diseases. Notification must be made to the Communicable Disease Control Branch of SA Health as soon as possible and at least within three days of suspicion of diagnosis, by telephone or post.
Route of transmission
> Infection with chickenpox is transmitted through airborne / respiratory droplets and direct contact with vesicle fluid
Incubation period
> 10 to 21 days (may be up to 35 days in contacts given high titre zoster immunoglobulin, ZIG)
Period of infectivity
> 48 hours before the onset of rash until crusting of all lesions (usually day 6 of rash)
> Infectious period may be prolonged in people with impaired immunity
Infection Control
> Non-immune staff should not care for the woman / baby infected with chickenpox
> Varicella (and herpes zoster) vesicles contain large numbers of virus particles. Ensure appropriate transmission based (standard, contact and airborne) precautions including:
> A negative pressure room with door shut (chickenpox and disseminated shingles)
> Immune staff in attendance
> Gloves, gown
> All dressing materials should be treated as medical waste
> Chickenpox and disseminated shingles use standard, contact and airborne precautions
> Localized shingles use contact precautions (only immune staff in attendance, single room, gloves, gown)
> In herpes zoster (shingles), transmission of infection usually requires contact with vesicle fluid; however, there is also evidence of respiratory spread. Localized shingles requires standard and contact precautions (not airborne precautions)
Susceptibility to varicella
> Women and babies susceptible to infection with VZV (may be severe or life-threatening) include:
> No history of varicella (chickenpox or shingles)
> Seronegative for varicella antibodies (VZV-IgG negative)
> No documented evidence of varicella vaccination
Significant Exposure
> For the purpose of infection control and prophylaxis, significant exposure of a susceptible woman who is pregnant to varicella includes:
> Living in the same household as a person with active varicella or herpes zoster
OR
> Direct face to face contact with a person with varicella or herpes zoster for at least 5 minutes
OR
> Being in the same room for at least 1 hour
> Chickenpox cases are infectious from 2 days before rash until lesions crusted
Management of maternal exposure to varicella-zoster virus
History of previous chickenpox
> No action required
No or uncertain history of chickenpox
> Obtain serology for antibody status (VZV-IgG) (if practicable)
> ZIG if required should be given within 96 hours. Testing should only be done if ZIG would still be able to be given, if required, within this window
Within 96 hours from exposure
> Zoster immunoglobulin (ZIG) should be given to all seronegative women within 96 hours (see adult dose under ZIG dosage below)
> However there may be some limited effect out to as late as 10 days post exposure
> Advise to seek medical care immediately if chickenpox develops
More than 96 hours following exposure
> Oral aciclovir or valaciclovir (see dosage below) should be considered for women:
> In the second half of pregnancy
> With a history of an underlying lung disease
> Who are immuno-compromised
> Who are smokers
Note: First make sure that you set up a monitor to keep track of the infected person, click here to find out how. Also, advise women to seek medical care immediately if chickenpox develops
Management of varicella-zoster in pregnancy
Less than 24 hours since appearance of rash
> Oral aciclovir 800 mg 5 times a day for 7 days OR oral valaciclovir 1 g three times a day for 7 days]
> Monitor at home
More than 24 hours since onset of rash
> No oral aciclovir / valaciclovir and monitor at home if:
> No underlying lung disease
> Not immunocompromised
> Non-smoker
> Monitor in hospital if any of the above risk factors
> No perinatal physiotherapy or postnatal physiotherapy until symptoms clear
> Offer appropriate fetal medicine counselling
Complications
> Advise to seek medical attention for the following complications:
> Respiratory symptoms
> Haemorrhagic rash or bleeding
> New pocks developing after 6 days
> Persistent fever
> 6 days
> Neurological symptoms
> Give aciclovir 10 mg / kg every 8 hours for 7 to 10 days (IV followed by oral [see dosage below]) and administer supportive therapy
Consider caesarean section if:
> Signs of significant fetal compromise
> Evidence of maternal respiratory failure exacerbated by advanced
Risk of fetal varicella syndrome (FVS) after maternal VZV
Timing of maternal infection:
>Less than 12 weeks gestation- 0.55%
>12-28 weeks gestation- 1.4%
>More than 28 weeks gestation- No cases of FVS reported
Refer to maternal fetal specialist for prenatal diagnosis and counselling
> Detailed fetal ultrasound for anomalies is recommended at least five weeks after primary infection
> Repeat ultrasounds until delivery. If abnormal may consider fetal MRI
> VZV fetal serology is unhelpful
> Amniocentesis not routinely advised if ultrasound normal, because risks of FVS low but negative VZV PCR may be reassuring
Management of infants exposed to maternal varicella zoster
Maternal chickenpox > 7 days before delivery
> No zoster immunoglobulin (ZIG) required
> No isolation required
> Encourage breastfeeding
> No other interventions even if baby has chickenpox at or very soon after birth unless preterm < 28 weeks gestation or low birth weight < 1,000 g > Very preterm infants (≤ 28 weeks gestation) born with chickenpox should receive intravenous aciclovir 20 mg / kg / dose every 8 hours as a slow infusion (1-2 hours)
Thank you to Christine DeFranco PGY-4 EM Resident for this review of VZV in pregnancy!